Abstract
Purpose
Regular surveillance decreases the risk of recurrent cancer in colorectal cancer (CRC) survivors. However, studies suggest that receipt of follow-up tests is not consistent with guidelines. This systematic review aimed to: (1) examine receipt of recommended post-treatment surveillance tests and procedures among CRC survivors, including adherence to established guidelines, and (2) identify correlates of CRC surveillance.
Methods
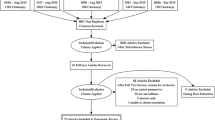
Systematic searches of Medline, PubMed, PsycINFO, CINAHL Plus, and Scopus databases were conducted using terms adapted for each database’s keywords and subject headings. Studies were screened for inclusion using a three-step process: (1) lead author reviewed abstracts of all eligible studies; (2) coauthors reviewed random 5 % samples of abstracts; and (3) two sets of coauthors reviewed all “maybe” abstracts. Discrepancies were adjudicated through discussion.
Results
Thirty-four studies are included in the review. Overall adherence ranged from 12 to 87 %. Within the initial 12 to 18 months post-treatment, adherence to recommended office visits was 93 %. Adherence ranged from 78 to 98 % for physical exams, 18–61 % for colonoscopy, and 17–71 % for carcinoembryonic antigen (CEA) testing. By 2 to 3 years post-treatment, cumulative adherence ranged from 70 to 88 % for office visits, 89–93 % for physical exams, 49–94 % for colonoscopy, and 7–79 % for CEA testing. Between 18 and 28 % of CRC survivors received greater than recommended overall surveillance; overuse of physical exams (42 %), colonoscopy (24–76 %), and metastatic disease testing (1–29 %) was also prevalent. Studies of correlates of CRC surveillance focused on sociodemographic and disease/treatment characteristics, and patterns of association were inconsistent across studies.
Conclusions
Deviation from surveillance recommendations includes both under- and overuse. Examination of modifiable determinants is needed to inform interventions targeting appropriate and timely receipt of recommended surveillance.
Implications for Cancer Survivors
Among CRC survivors, it remains unclear what modifiable psychosocial factors are associated with the observed under- and overuse of surveillance. Understanding and intervening with these psychosocial factors is critical to improving adherence to guideline-recommended surveillance and thereby reducing mortality among this group of survivors.

Similar content being viewed by others
References
American Cancer Society. Cancer facts & figures 2012. Atlanta: American Cancer Society; 2012.
Hu C-Y, Delclos GL, Chan W, et al. Post-treatment surveillance in a large cohort of patients with colon cancer. Am J Manag Care. 2011;17:329–36.
Hammond K, Margolin DA. The role of postoperative surveillance in colorectal cancer. Clin Colon Rectal Surg. 2007;20:249–54.
Obrand DI, Gordon PH. Incidence and patterns of recurrence following curative resection for colorectal carcinoma. Dis Colon Rectum. 1997;40:15–24.
Tjandra JJ, Chan MKY. Follow-up after curative resection of colorectal cancer: a meta-analysis. Dis Colon Rectum. 2007;50:1783–99.
Renehan AG, Egger M, Saunders MP, et al. Impact on survival of intensive follow-up after curative resection for colorectal cancer: systematic review and meta-analysis of randomised trials. BMJ. 2002;324:1–8.
Figueredo A, Rumble RB, Maroun J, et al. Follow-up of patients with curatively resected colorectal cancer: a practice guideline. BMC Cancer. 2003;3:26.
Kunitake H, Zheng P, Land SR, et al. Routine preventive care and cancer surveillance in long-term survivors of colorectal cancer: results from National Surgical Adjuvant Breast and Bowel Project Protocol LTS-01. J Clin Oncol. 2010;28:5274–9.
Anthony T, Simmang C, Hyman N, et al. Practice parameters for the surveillance and follow-up of patients with colon and rectal cancer. Dis Colon Rectum. 2004;47:807–17.
American Cancer Society. Colorectal cancer detailed guide; 6-17-2011. Available at: http://www.cancer.org/Cancer/ColonandRectumCancer/DetailedGuide/index. Accessed 17 June 2011.
Rex DK, Kahi CJ, Levin B, et al. Guidelines for colonoscopy surveillance after cancer resection: a consensus update by the American Cancer Society and the US Multi-Society Task Force on Colorectal Cancer. Gastroenterology. 2006;130:1865–71.
Desch CE, Benson AB, Somerfield MR, et al. Colorectal cancer surveillance: 2005 update of an American Society of Clinical Oncology practice guideline. J Clin Oncol. 2005;23:8512–9.
National Comprehensive Cancer Network. NCCN clinical practice guidelines in oncology: colon cancer, version 1. 2011; 8-30-2011.
Jeffery M, Hickey BE, Hider PN. Follow-up strategies for patients treated for non-metastatic colorectal cancer. Cochrane Database Syst Rev. 2007; CD002200.
Boehmer U, Harris J, Bowen DJ, et al. Surveillance after colorectal cancer diagnosis in a safety net hospital. J Health Care Poor Underserved. 2010;21:1138–51.
Borie F, Daures J-P, Millat B. Cost and effectiveness of follow-up examinations in patients with colorectal cancer resected for cure in a French population-based study. J Gastrointest Surg. 2004;8:552–8.
Boulin M, Lejeune C, Le Teuff G, et al. Patterns of surveillance practices after curative surgery for colorectal cancer in a French population. Dis Colon Rectum. 2005;48:1890–9.
Brawarsky P, Neville BA, Fitzmaurice GM, et al. Surveillance after resection for colorectal cancer. Cancer. 2013;119:1235–42.
Cardella J, Coburn NG, Gagliardi A. Compliance, attitudes and barriers to post-operative colorectal cancer follow-up. J Eval Clin Pract. 2008;14:407–15.
Cheung WY, Pond GR, Rother M, et al. Adherence to surveillance guidelines after curative resection for stage II/III colorectal cancer. Clin Colorectal Canc. 2008;7:191–6.
Cooper GS, Yuan Z, Chak A, et al. Geographic and patient variation among Medicare beneficiaries in the use of follow-up testing after surgery for nonmetastatic colorectal carcinoma. Cancer. 1999;85:2124–31.
Cooper GS, Yuan Z, Chak A, et al. Patterns of endoscopic follow-up after surgery for nonmetastatic colorectal cancer. Gastrointest Endosc. 2000;52:33–8.
Cooper GS, Payes JD. Temporal trends in colorectal procedure use after colorectal cancer resection. Gastrointest Endosc. 2006;64:933–40.
Cooper GS, Kou TD, Reynolds HL. Receipt of guideline-recommended follow-up in older colorectal cancer survivors. Cancer. 2008;113:2029–37.
Ellison GL, Warren JL, Knopf KB, et al. Racial differences in the receipt of bowel surveillance following potentially curative colorectal cancer surgery. Health Serv Res. 2003;38:1885–904.
Elston Lafata J, Johnson CC, Ben-Menaghem T, et al. Sociodemographic differences in the receipt of colorectal cancer surveillance care following treatment with curative intent. Med Care. 2001;39:361–72.
Elston Lafata J, Simpkins J, Schultz L, et al. Routine surveillance care after cancer treatment with curative intent. Med Care. 2005;43:592–9.
Foley KL, Song E-Y, Klepin H, et al. Screening colonoscopy among colorectal cancer survivors insured by Medicaid. Am J Clin Oncol. 2011;35:205–11.
Fox JP, Jeffery DD, Williams TV, et al. Quality of cancer survivorship care in the military health system (TRICARE). Cancer J. 2013;19:1–9.
Haggstrom DA, Arora NK, Helft P, et al. Follow-up care delivery among colorectal cancer survivors most often seen by primary and subspecialty care physicians. J Gen Intern Med. 2009;24:472–9.
Hilsden RJ, Bryant HE, Sutherland LR, et al. A retrospective study on the use of post-operative colonoscopy following potentially curative surgery for colorectal cancer in a Canadian province. BMC Cancer. 2004;4:14.
Jackson GL, Melton D, Abbot DH, et al. Quality of nonmetastatic colorectal cancer care in the Department of Veterans Affairs. J Clin Oncol. 2010;28:3176–81.
Knopf KB, Warren JL, Feuer EJ, et al. Bowel surveillance patterns after a diagnosis of colorectal cancer in Medicare beneficiaries. Gastrointest Endosc. 2001;54:563–71.
Parsons HM, Tuttle TM, Kuntz KM, et al. Quality of care along the cancer continuum: Does receiving adequate lymph node evaluation for colon cancer lead to comprehensive postsurgical care? J Am Coll Surg. 2012; doi:10.1016/j.jamcollsurg.2012.05.014
Pollack LA, Adamache W, Ryerson AB, et al. Care of long-term cancer survivors: physicians seen by Medicare enrollees surviving longer than 5 years. Cancer. 2009;115:5284–95.
Ramsey SD, Howlader N, Etzioni R, et al. Surveillance endoscopy does not improve survival for patients with local and regional stage colorectal cancer. Cancer. 2007;109:2222–8.
Rolnick S, Alford SH, Kucera GP, et al. Racial and age differences in colon examination surveillance following a diagnosis of colorectal cancer. J Natl Cancer Inst Monogr. 2005;35:96–101.
Rulyak SJ, Madelson MT, Brentnall TA, et al. Clinical and sociodemographic factors associated with colon surveillance among patients with a history of colorectal cancer. Gastrointest Endosc. 2004;59:239–47.
Rulyak SJ, Lieberman DA, Wagner EH, et al. Outcome of follow-up colon examination among a population-based cohort of colorectal cancer patients. Clin Gastroenterol H. 2007;5:470–6.
Salloum RG, Hornbrook MC, Fishman PA, et al. Adherence to surveillance care guidelines after breast and colorectal cancer treatment with curative intent. Cancer. 2012. doi:10.1002/cncr.27544.
Salz T, Weinberger M, Ayanian JZ, et al. Variation in use of surveillance colonoscopy among colorectal cancer survivors in the United States. BMC Health Serv Res. 2010;10:256–63.
Singh A, Kuo Y-F, Goodwin JS. Many patients who undergo surgery for colorectal cancer receive surveillance colonoscopies earlier than recommended by guidelines. Clin Gastroenterol H. 2013;11:65–72.
Sisler JJ, Seo B, Katz A, et al. Concordance with ASCO guidelines for surveillance after colorectal cancer treatment: a population-based analysis. J Oncol Pract. 2012;8:e69–79.
Spratlin JL, Hui D, Hanson J, et al. Community compliance with carcinoembryonic antigen: follow-up of patients with colorectal cancer. Clin Colorectal Canc. 2008;7:118–25.
Earle CC, Neville BA. Under use of necessary care among cancer survivors. Cancer. 2004;101:1712–9.
Mahboubi A, Lejeune C, Coriat R, et al. Which patients with colorectal cancer are followed up by general practitioners? A population-based study. Eur J Cancer Prev. 2007;16:535–41.
Sabatino SA, Thompson TD, Smith JL, et al. Receipt of cancer treatment summaries and follow-up instructions among adult cancer survivors: results from a national survey. J Cancer Surviv. 2013;7:32–43.
Treanor C, Donnelly M. An international review of the patterns and determinants of health service utilization by adult cancer survivors. BMC Health Serv Res. 2012;12:316.
Salz T, Woo H, Starr TD, et al. Ethnic disparities in colonoscopy use among colorectal cancer survivors: a systematic review. J Cancer Surviv. 2012;6:372–8.
Vandenbroucke JP, von Elm E, Altman DG, et al. Strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. PLos Med. 2007;4:e297.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med. 2009;151:65–94.
Higgins JPT, Green S. Cochrane handbook for systematic reviews of interventions. Chichester: Wiley; 2008.
Klabunde CN, Cronin KA, Breen N, et al. Trends in colorectal cancer test use among vulnerable populations in the United States. Cancer Epidemiol Biomarkers Prev. 2011;20:1611–21.
Potosky AL, Han PKJ, Rowland J, et al. Differences between primary care physicians’ and oncologists’ knowledge, attitudes and practices regarding the care of cancer survivors. J Gen Intern Med. 2011;26:1403–10.
Vernon SW, McQueen A. Colorectal cancer screening. In: Holland JC et al., editors. Psycho-oncology. 2nd ed. New York: Oxford University Press; 2010. p. 71–83.
Salz T, Brewer NT, Sandler RS, et al. Association of health beliefs and colonoscopy use among survivors of colorectal cancer. J Cancer Surviv. 2009;3:193–201.
Taplin SH, Price RA, Edwards HM, et al. Introduction: understanding and influencing multilevel factors across the cancer care continuum. J Natl Cancer Inst Monogr. 2012;2012:2–10.
National Cancer Institute. Understanding and influencing multilevel factors across the cancer care continuum. J Natl Cancer Inst Monogr. 2012;2012:1–134.
The COMMIT Research Group. Community intervention trial for smoking cessation (COMMIT): II. Changes in adult cigarette smoking prevalence. Am J Public Health. 1995;85:193–200.
Lytle LA, Stone EJ, Nichaman MZ, et al. Changes in nutrient intakes of elementary school children following a school-based intervention: results from the CATCH study. Prev Med. 1996;25:465–77.
Lorig KR, Holman HR. Self-management education: history, definition, outcomes, and mechanisms. Ann Behav Med. 2003;26:1–7.
Cimprich B, Janz NK, Northouse L, et al. Taking charge: a self-management program for women following breast cancer treatment. Psychooncology. 2005;14:704–17.
Damush TM, Perkins A. The implementation of an oncologist referred, exercise self-management program for older breast cancer survivors. Psychooncology. 2006;15:884–90.
Stanton AL. Psychosocial concerns and interventions for cancer survivors. J Clin Oncol. 2008;24:5132–7.
Grunfeld E. Primary care physicians and oncologists are players on the same team. J Clin Oncol. 2008;26:2246–7.
Hudson MM, Landier W, Ganz PA. Impact of survivorship-based research on defining clinical care guidelines. Cancer Epidemiol Biomarkers Prev. 2011;20:2085–92.
Grunfeld E, Mant D, Yudkin P, et al. Routine follow up of breast cancer in primary care: randomised trial. BMJ. 1996;313:665–9.
Grunfeld E, Levine MN, Julian JA, et al. Randomized trial of long-term follow-up for early stage breast cancer: a comparison of family physician versus specialist care. J Clin Oncol. 2006;24:848–55.
Wattchow DA, Weller DP, Esterman A, et al. General practice vs surgical-based follow-up for patients with colon cancer: randomised controlled trial. Br J Cancer. 2006;94:1116–21.
Del Giudice M, Grunfeld E, Harvey BJ, et al. Primary care physicians’ views of routine follow-up care of cancer survivors. J Clin Oncol. 2009;27:3338–45.
Steckler A, McLeroy KR. The importance of external validity. Am J Public Health. 2008;98:9–10.
Acknowledgments
The authors would like to thank Helena Vonville, MLS for her assistance in developing the search strategy. This work was supported by the National Cancer Institute at the National Institutes of Health (K07CA140159 to M.Y.C. and R01CA112223 to S.W.V.) and the Susan G. Komen Foundation (KG111378 to S.M.B.). S.M.B. was also supported by the Cancer Education and Career Development Program at the School of Public Health, University of Texas Health Science Center at Houston, funded by the National Cancer Institute (R25T 2R25CA57712). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Cancer Institute, the National Institutes of Health, or the Susan G. Komen Foundation.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Search strategy for Ovid Medline
-
1.
exp Colorectal neoplasms/
-
2.
(crc or ((colorectal or colon or rectal) adj3 (cancer* or neoplasm* or polyp*))).ti,ab.
-
3.
1 or 2
-
4.
Survivors/ or survivor*.ti,ab.
-
5.
3 and 4
-
6.
Mass screening/
-
7.
screen*.ti,ab.
-
8.
surveillance.ti,ab. or follow-up.ti,ab.
-
9.
exp Colonoscopy/
-
10.
exp Sigmoidoscopy/
-
11.
exp Endoscopy/
-
12.
Barium enema.ti,ab.
-
13.
Occult blood/
-
14.
or/6–13
-
15.
5 and 14
-
16.
Limit 15 to English language
Search strategy for PubMed
-
1.
Colorectal neoplasms[mesh0]
-
2.
(crc[tiab] OR colorectal[tiab] OR colon[tiab] OR rectal[tiab] AND (cancer*[tiab] OR neoplasm*[tiab] OR polyp*[tiab])
-
3.
#1 OR #2
-
4.
Survivors[mesh:noexp] OR survivor*[tiab]
-
5.
#3 AND #4
-
6.
Mass screening[mesh:noexp]
-
7.
Screen*[tiab]
-
8.
Surveillance[tiab] OR follow-up[tiab]
-
9.
Colonoscopy[mesh]
-
10.
Sigmoidoscopy[mesh]
-
11.
Endoscopy[mesh]
-
12.
Barium enema[tiab]
-
13.
Occult blood[mesh:noexp]
-
14.
#6 OR #7 OR #8 OR #9 OR #10 OR #11 OR #12 OR #13
-
15.
#5 AND #14
-
16.
#5 AND #14 Filters: English
Search strategy for Ovid PsycINFO
-
1.
Colorectal neoplasms/
-
2.
((crc or colorectal or colon or rectal) adj4 (cancer* or neoplasm* or polyp*)).ti,ab,id.
-
3.
1 or 2
-
4.
Survivors/ or survivor*.ti,ab,id.
-
5.
3 and 4
-
6.
Mass screening.md.
-
7.
Screen*.ti,ab,id.
-
8.
Surveillance.ti,ab,id. or follow-up.ti,ab,id.
-
9.
Colonoscopy/
-
10.
Sigmoidoscopy/
-
11.
Endoscopy/
-
12.
Barium enema.ti,ab,id.
-
13.
Occult blood/
-
14.
or/6–13
-
15.
5 and 14
-
16.
Limit 15 to English language
Search strategy for CINAHL
-
1.
(MH “Colorectal Neoplasms”)
-
2.
TI ( (crc or colorectal or colon or rectal) and (cancer* or neoplasm* or polyp*) ) or AB ( (crc or colorectal or colon or rectal) and (cancer* or neoplasm* or polyp*) )
-
3.
S1 or S2
-
4.
(MH “Survivors”)
-
5.
TI survivor* or AB survivor*
-
6.
S4 or S5
-
7.
S3 and S6
-
8.
Mass screening/
-
9.
TI screen* or AB screen*
-
10.
TI (surveillance or follow-up) or AB (surveillance or follow-up)
-
11.
(MH “Colonoscopy”)
-
12.
(MH “Sigmoidoscopy”)
-
13.
(MH “Endoscopy”)
-
14.
TI barium enema or AB barium enema
-
15.
Occult blood/
-
16.
S8 or S9 or S10 or S11 or S12 or S13 or S14 or S15
-
17.
S7 and S16
-
18.
S7 and S16 limiters—English language
Rights and permissions
About this article
Cite this article
Carpentier, M.Y., Vernon, S.W., Bartholomew, L.K. et al. Receipt of recommended surveillance among colorectal cancer survivors: a systematic review. J Cancer Surviv 7, 464–483 (2013). https://doi.org/10.1007/s11764-013-0290-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-013-0290-x