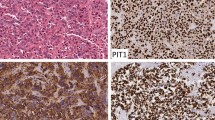
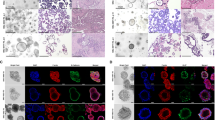
Abstract
Neuroendocrine tumors (NETs) represent a heterogeneous group of diseases with varied natural history and prognosis depending upon the organ of origin and grade of aggressiveness. The most widely used biomarker to determine disease burden and monitor response to treatment is chromogranin A (CgA), but it is far from being the optimal predictive and prognostic biomarker in NETs. Biological understanding and derived treatment options for NETs have changed markedly in recent years. Over the last decade, the genomic landscape of these tumors has been extensively investigated. This has resulted in the discovery of mutations and expression anomalies in genes and pathways such as the PI3K/Akt/mTOR, DAXX/ATRX, and MEN1, which are promising predictive and prognostic biomarkers and future candidates for targeted therapies. Additionally, the study of tumor stroma and environment are one of the most promising fields for discovery of potential new targets and biomarkers.
Similar content being viewed by others
References
Aaltonen, L.A., Hamilton, S.R., World Health Organization., International Agency for Research on Cancer. Pathology and genetics of tumours of the digestive system. Lyon Oxford: IARC Press; Oxford University Press; 2000.
Rindi, G., Kloppel, G., Alhman, H., et al. (2006). TNM staging of foregut (neuro)endocrine tumors: a consensus proposal including a grading system. Virchows Archiv, 449, 395–401.
Rindi, G., Kloppel, G., Couvelard, A., et al. (2007). TNM staging of midgut and hindgut (neuro) endocrine tumors: a consensus proposal including a grading system. Virchows Archiv, 451, 757–762.
Kloppel, G., Rindi, G., Perren, A., Komminoth, P., & Klimstra, D. S. (2010). The ENETS and AJCC/UICC TNM classifications of the neuroendocrine tumors of the gastrointestinal tract and the pancreas: a statement. Virchows Archiv, 456, 595–597.
Bosman, F. T. (2010). World Health Organization, International Agency for Research on Cancer. WHO classification of tumours of the digestive system (4th ed.). Lyon: International Agency for Research on Cancer.
Rinke, A., Müller, H. H., Schade-Brittinger, C., et al. (2009). Placebo-controlled, double-blind, prospective, randomized study on the effect of octreotide LAR in the control of tumor growth in patients with metastatic neuroendocrine midgut tumors: a report from the PROMID study group. Journal of Clinical Oncology, 27, 4656–63.
Caplin, M., Ruszniewski, P., Pavel, M., et al. (2013). A randomized, double-blind, placebo-Controlled study of lanreotide antiproliferative response in patients with gastroenteropancreatic NeuroEndocrine Tumors (CLARINET). EJC 47 (Suppl.2): abstract 8961.
Oberg, K. E., Casanovas, O., Castano, J. P., Chung, D., Dell Fave, G., Denèfle, P., et al. (2013). Molecular pathogenesis of neuroendocrine tumors: implications for current and future therapeutic approaches. Clinical Cancer Research, 19, 2842–2849.
Durán-Prado, M., Saveanu, A., Luque, R. M., et al. (2010). A potential inhibitory role for the new truncated variant of somatostatin receptor 5, sst5TMD4, in pituitary adenomas poorly responsive to somatostatin analogs. Journal of Clinical Endocrinology and Metabolism, 95, 2497–502.
Jones, S., Zhang, X., Parsons, D. W., et al. (2008). Core signaling pathways in human pancreatic cancers revealed by global genomic analyses. Science, 321, 1801–6.
de Wilde, R. F., Edil, B. H., Hruban, R. H., & Maitra, A. (2012). Well-differentiated pancreatic neuroendocrine tumors: from genetics to therapy. Nature Reviews Gastroenterology & Hepatology, 9, 199–208.
Corbo, V., Dalai, I., Scardoni, M., Barbi, S., Beghelli, S., Bersani, S., et al. (2010). MEN1 in pancreatic endocrine tumors: analysis of gene and protein status in 169 sporadic neoplasms reveals alterations in the vast majority of cases. Endocrine-Related Cancer, 17, 771–83.
Heaphy, C. M., de Wilde, R. F., Jiao, Y., et al. (2011). Altered telomeres in tumors with ATRX and DAXX mutations. Science, 333, 425.
de Wilde, R. F., Heaphy, C. M., Maitra, A., et al. (2012). Loss of ATRX or DAXX expression and concomitant acquisition of the alternative lengthening of telomeres phenotype are late events in a small subset of MEN-1 syndrome pancreatic neuroendocrine tumors. Modern Pathology, 25, 1033–9.
Cingarlini, S., Bonomi, M., Corbo, V., Scarpa, A., & Tortora, G. (2012). Profiling mTOR pathway in neuroendocrine tumors. Targeted Oncology, 7, 183–8.
Missiaglia, E., Dalai, I., Barbi, S., et al. (2010). Pancreatic endocrine tumors: expression profiling evidences a role for AKT-mTOR pathway. Journal of Clinical Oncology, 28, 245–55.
Yao, J. C., Shah, M. H., Ito, T., et al. (2011). Everolimus for advanced pancreatic neuroendocrine tumors. New England Journal of Medicine, 364, 514–23.
Yachida, S., Jones, S., Bozic, I., et al. (2010). Distant metastasis occurs late during the genetic evolution of pancreatic cancer. Nature, 467, 1114–7.
Volinia, S., Calin, G. A., Liu, C. G., et al. (2006). A microRNA expression signature of human solid tumors defines cancer gene targets. Proceedings of the National Academy of Sciences of the United States of America, 103, 2257–61.
Roldo, C., Missiaglia, E., Hagan, J. P., et al. (2006). MicroRNA expression abnormalities in pancreatic endocrine and acinar tumors are associated with distinctive pathologic features and clinical behavior. Journal of Clinical Oncology, 24, 4677–84.
Li, S. C., Essaghir, A., Martijn, C., Lloyd, R. V., Demoulin, J. B., Oberg, K., et al. (2013). Global microRNA profiling of well-differentiated small intestinal neuroendocrine tumors. Modern Pathology, 26, 685–96.
Modlin, I. M., et al. (2010). A nomogram to assess small-intestinal neuroendocrine tumor (‘carcinoid’) survival. Neuroendocrinology, 92, 143–157.
Vinik, E., Carlton, C. A., Silva, M. P., & Vinik, A. I. (2009). Development of the Norfolk quality of life tool for assessing patients with neuroendocrine tumors. Pancreas, 38, e87–95.
Taupenot, L., Harper, K. L., & O’Connor, D. T. (2003). The chromogranin-secretogranin family. New England Journal of Medicine, 348, 1134–1149.
Yao, J. C., Pavel, M., Phan, A. T., Kulke, M. H., Hoosen, S., St Peter, J., et al. (2011). Chromogranin a and neuron-specific enolase as prognostic markers in patients with advanced pNET treated with everolimus. Journal of Clinical Endocrinology and Metabolism, 96, 3741–3749.
Yao, J. C., Phan, A. T., Chang, D. Z., Wolf, R. A., Hess, K., Gupta, S., et al. (2008). Efficacy of RAD001 (everolimus) and octreotide LAR in advanced low- to intermediate-grade neuroendocrine tumors: results of a phase II study. Journal of Clinical Oncology, 26, 4311–4318.
Yao, J. C., Lombard-Dohas, C., Baudin, E., Kvols, L. K., Rougier, P., Ruszniwski, P., et al. (2010). Daily oral everolimus activity in patients with metastatic pancreatic neuroendocrine tumors after failure of cytotoxic chemotherapy: a phase II trial. Journal of Clinical Oncology, 28, 69–76.
Marotta, V., Nuzzo, V., Ferrara, T., Zuccoli, A., Masone, M., Nocerino, L., et al. (2012). Limitations of chromogranin A in clinical practice. Biomarkers, 17, 186–191.
Campana, D., et al. (2007). Chromogranin A: is it a useful marker of neuroendocrine tumors? Journal of Clinical Oncology, 25, 1967–1973.
Capdevila, J., & Tabernero, J. (2011). A shining light in the darkness for the treatment of pancreatic neuroendocrine tumors. Cancer Discovery, 1, 213–221.
Bello, C., et al. (2006). Analysis of circulating biomarkers of sunitinib maleate in patients with unresectable neuroendocrine tumors (NET): VEGF, IL-8, and soluble VEGF receptors 2 and 3. American Society of Clinical Oncology, 24, 4045.
Grande, E., Casanovas, O., Earl, J, et al. (2013). sVEGFR2 and circulating tumor cells to predict for the efficacy of pazopanib in neuroendocrine tumors (NETs): PAZONET subgroup analysis. J Clin Oncol 31; suppl: abstr 4140.
Raymond, E., et al. (2011). Sunitinib malate for the treatment of pancreatic neuroendocrine tumors. New England Journal of Medicine, 364, 501–513.
Kulke, M. H., et al. (2009). O6-methylguanine DNA methyltransferase deficiency and response to temozolomide-based therapy in patients with neuroendocrine tumors. Clinical Cancer Research, 15, 338–345.
Modlin, I. M., et al. (2008). Gastroenteropancreatic neuroendocrine tumors. Lancet Oncology, 9, 61–72.
Cui, T., et al. (2010). Paraneoplastic antigen Ma2 autoantibodies as specific blood biomarkers for detection of early recurrence of small intestine neuroendocrine tumors. PLoS One, 5, e16010.
Khan, M. S., et al. (2013). Circulating tumor cells as prognostic markers in neuroendocrine tumors. Journal of Clinical Oncology, 31, 365–372.
Chan, J. A., et al. (2012). Prospective study of bevacizumab plus temozolomide in patients with advanced neuroendocrine tumors. Journal of Clinical Oncology, 30, 2963–2968.
Raymond, E., et al. (2011). Sunitinib malate for the treatment of pancreatic neuroendocrine tumors. New England Journal of Medicine, 364, 501–513.
Pavel, M. E., et al. (2011). Everolimus plus octreotide long-acting repeatable for the treatment of advanced neuroendocrine tumors associated with carcinoid syndrome (RADIANT-2): a randomised, placebo-controlled, phase 3 study. Lancet, 378, 2005–2012.
Yao, J. C., et al. (2008). Targeting vascular endothelial growth factor in advanced carcinoid tumor: a random assignment phase II study of depot octreotide with bevacizumab and pegylated interferon alpha-2b. Journal of Clinical Oncology, 26, 1316–1323.
Binderup, T., Knigge, U., Loft, A., Federspiel, B., & Kjaer, A. (2010). 18F-fluorodeoxyglucose positron emission tomography predicts survival of patients with neuroendocrine tumors. Clinical Cancer Research, 16, 978–985.
Pietras, K., & Ostman, A. (2010). Hallmarks of cancer: interactions with the tumor stroma. Experimental Cell Research, 316, 1324–1331.
Hanahan, D. (1985). Heritable formation of pancreatic beta-cell tumors in transgenic mice expressing recombinant insulin/simian virus 40 oncogenes. Nature, 315, 115–122.
Paez-Ribes, M., et al. (2009). Antiangiogenic therapy elicits malignant progression of tumors to increased local invasion and distant metastasis. Cancer Cell, 15, 220–231.
Chiu, C. W., Nozawa, H., & Hanahan, D. (2010). Survival benefit with proapoptotic molecular and pathologic responses from dual targeting of mammalian target of rapamycin and epidermal growth factor receptor in a preclinical model of pancreatic neuroendocrine carcinogenesis. Journal of Clinical Oncology, 28, 4425–4433.
Yao, J. C., et al. (2011). Everolimus for advanced pancreatic neuroendocrine tumors. New England Journal of Medicine, 364, 514–523.
Gerhardt, H., & Betsholtz, C. (2003). Endothelial-pericyte interactions in angiogenesis. Cell and Tissue Research, 314, 15–23.
Pietras, K., & Hanahan, D. A. (2005). Multitargeted, metronomic, and maximum-tolerated dose “chemo-switch” regimen is antiangiogenic, producing objective responses and survival benefit in a mouse model of cancer. Journal of Clinical Oncology, 23, 939–952.
Cunha, S. I., et al. (2010). Genetic and pharmacological targeting of activin receptor-like kinase 1 impairs tumor growth and angiogenesis. Journal of Experimental Medicine, 207, 85–100.
Bellmunt, J., et al. (2010). Activity of a multitargeted chemo-switch regimen (sorafenib, gemcitabine, and metronomic capecitabine) in metastatic renal-cell carcinoma: a phase 2 study (SOGUG-02-06). Lancet Oncology, 11, 350–357.
Franco, M., Roswall, P., Cortez, E., Hanahan, D., & Pietras, K. (2011). Pericytes promote endothelial cell survival through induction of autocrine VEGF-A signaling and Bcl-w expression. Blood, 118, 2906–2917.
Franco, M., Paez-Ribes, M., Cortez, E., Casanovas, O., & Pietras, K. (2011). Use of a mouse model of pancreatic neuroendocrine tumors to find pericyte biomarkers of resistance to anti-angiogenic therapy. Hormone and Metabolic Research, 43, 884–889.
Cunha, S. I., & Pietras, K. (2011). ALK1 as an emerging target for antiangiogenic therapy of cancer. Blood, 117, 6999–7006.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Capdevila, J., Meeker, A., García-Carbonero, R. et al. Molecular biology of neuroendocrine tumors: from pathways to biomarkers and targets. Cancer Metastasis Rev 33, 345–351 (2014). https://doi.org/10.1007/s10555-013-9468-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10555-013-9468-y