Abstract
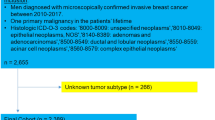
Substantial controversy exists about the prognostic role of tumor subtypes in male breast cancer (MaBC). The aim of this study was to analyze the characteristics of each tumor subtype in MaBC and its association with prognosis compared with other factors. We evaluated MaBC patients between 2010 and 2012 with known estrogen receptor, progesterone receptor [together hormone receptor (HR)] status, and human epidermal growth factor receptor 2 (HER2) status reported to the Surveillance, Epidemiology, and End Results program. Patients were classified as: HR-positive/HER2-negative, HR-positive/HER2-positive, HR-negative/HER2-positive, and triple-negative (TN). Univariate and multivariate analyses determined the effect of each variable on overall survival (OS). We included 960 patients. Patient distribution was 84.9 % HR-positive/HER2-negative, 11.6 % HR-positive/HER2-positive, 0.6 % HR-negative/HER2-positive, and 2.9 % TN. TN patients were younger, had higher grade, presented with more advanced stage, were more likely to have mastectomy, and to die of breast cancer (all P < 0.05). Univariate analysis showed that HER2 positivity was associated with shorter OS (hazard ratio 1.90, P = 0.031) and TN patients had worse prognosis (hazard ratio 5.10, P = 0.0004). In multivariate analysis, older patients (hazard ratio 3.10, P = 0.032), those with stage IV (hazard ratio 16.27, P < 0.001) and those with TN tumors (hazard ratio 4.61, P = 0.002) had significantly worse OS. We observed significant differences in patient characteristics according to tumor subtype. HER2-positive and TN represented a small proportion of cases. In addition to age and stage, tumor subtype has clear influence on OS in MaBC.


Similar content being viewed by others
References
Giordano SH, Cohen DS, Buzdar AU, Perkins G, Hortobagyi GN (2004) Breast carcinoma in men: a population-based study. Cancer 101(1):51–57. doi:10.1002/cncr.20312
Anderson WF, Jatoi I, Tse J, Rosenberg PS (2010) Male breast cancer: a population-based comparison with female breast cancer. J Clin Oncol 28(2):232–239. doi:10.1200/JCO.2009.23.8162
Everson RB, Lippman ME, Thompson EB, McGuire WL, Wittliff JL, De Sombre ER, Jensen EV, Singhakowinta A, Brooks SC Jr, Neifeld JP (1980) Clinical correlations of steroid receptors and male breast cancer. Cancer Res 40(4):991–997
Sineshaw HM, Freedman RA, Ward EM, Flanders WD, Jemal A (2015) Black/white disparities in receipt of treatment and survival among men with early-stage breast cancer. J Clin Oncol. doi:10.1200/JCO.2014.60.5584
Chavez-Macgregor M, Clarke CA, Lichtensztajn D, Hortobagyi GN, Giordano SH (2013) Male breast cancer according to tumor subtype and race: a population-based study. Cancer 119(9):1611–1617. doi:10.1002/cncr.27905
Cardoso F, Bartlett J, Slaets L, van Deurzen C, van Leewen-Stok E, Porter P, Linderholm B, Hedenfalk I, Schroder C, Martens J (2015) (abstr S6-05) Characterization of male breast cancer: first results of the EORTC10085/TBCRC/BIG/NABCG International Male BC Program. Cancer Res 75(9 Supplement):S6-05
Arslan UY, Oksuzoglu B, Ozdemir N, Aksoy S, Alkis N, Gok A, Kaplan MA, Gumus M, Berk V, Uncu D, Baykara M, Colak D, Uyeturk U, Turker I, Isikdogan A (2012) Outcome of non-metastatic male breast cancer: 118 patients. Med Oncol 29(2):554–560. doi:10.1007/s12032-011-9978-9
Surveillance, Epidemiology, and End Results (SEER) Program (www.seer.cancer.gov) SEER*Stat Database: Incidence—SEER 18 Regs Research Data + Hurricane Katrina Impacted Louisiana Cases, Nov 2014 Sub (1973-2012 varying)—Linked To County Attributes—Total U.S., 1969-2013 Counties, National Cancer Institute, DCCPS, Surveillance Research Program, Surveillance Systems Branch, released April 2015, based on the November 2014 submission
Leach IH, Ellis IO, Elston CW (1992) c-erb-B-2 expression in male breast carcinoma. J Clin Pathol 45(10):942
Korde LA, Zujewski JA, Kamin L, Giordano S, Domchek S, Anderson WF, Bartlett JM, Gelmon K, Nahleh Z, Bergh J, Cutuli B, Pruneri G, McCaskill-Stevens W, Gralow J, Hortobagyi G, Cardoso F (2010) Multidisciplinary meeting on male breast cancer: summary and research recommendations. J Clin Oncol 28(12):2114–2122. doi:10.1200/JCO.2009.25.5729
Rudlowski C, Friedrichs N, Faridi A, Fuzesi L, Moll R, Bastert G, Rath W, Buttner R (2004) Her-2/neu gene amplification and protein expression in primary male breast cancer. Breast Cancer Res Treat 84(3):215–223. doi:10.1023/B:BREA.0000019953.92921.7e
Curigliano G, Colleoni M, Renne G, Mazzarol G, Gennari R, Peruzzotti G, de Braud E, Robertson C, Maiorano E, Veronesi P, Nole F, Mandala M, Ferretti G, Viale G, Goldhirsch A (2002) Recognizing features that are dissimilar in male and female breast cancer: expression of p21Waf1 and p27Kip1 using an immunohistochemical assay. Ann Oncol 13(6):895–902
Bloom KJ, Govil H, Gattuso P, Reddy V, Francescatti D (2001) Status of HER-2 in male and female breast carcinoma. Am J Surg 182(4):389–392
Muir D, Kanthan R, Kanthan SC (2003) Male versus female breast cancers. A population-based comparative immunohistochemical analysis. Arch Pathol Lab Med 127(1):36–41. doi:10.1043/0003-9985(2003)127<36:MVFB>2.0.CO;2
Giordano SH, Buzdar AU, Hortobagyi GN (2002) Breast cancer in men. Ann Intern Med 137(8):678–687
Rayson D, Erlichman C, Suman VJ, Roche PC, Wold LE, Ingle JN, Donohue JH (1998) Molecular markers in male breast carcinoma. Cancer 83(9):1947–1955
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Leone, J.P., Leone, J., Zwenger, A.O. et al. Prognostic significance of tumor subtypes in male breast cancer: a population-based study. Breast Cancer Res Treat 152, 601–609 (2015). https://doi.org/10.1007/s10549-015-3488-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-015-3488-y