Abstract
Purpose
The aim of this study was to clarify the changes in the cross-sectional area of skeletal muscle and muscle attenuation (MA) during 12-month period before death in breast cancer patients.
Methods
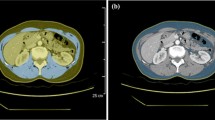
Breast cancer patients who received treatment between September 2002 and July 2014 at Shizuoka Cancer Center or between December 2005 and July 2014 at Teikyo University Hospital were identified. Computed tomography (CT) scans during the 12-month period before death of consecutive female patients who died of breast cancer were reviewed. Skeletal muscle quantity and quality were evaluated by a cross-sectional area of skeletal muscle and MA, respectively, on CT scans taken 10–12 months (T1), 7–9 months (T2), 4–6 months (T3), and within 3 months (T4) prior to death. Wilcoxon signed rank test was used to compare the differences between the two-time points with Bonferroni correction (p = 0.0083).
Results
The medical records of 99 patients (median age at death, 57 years; range, 40–83 years) were retrospectively analyzed. Both the cross-sectional area and MA continued to decrease during 12-month period before death. Statistically significant differences were observed in the cross-sectional areas between T1 and T4 (p = 0.0011), T2 and T4 (p = 0.0019), and T3 and T4 (p = 0.0026), as well as in MA between T2 and T4 (p = 0.0012) and T3 and T4 (p = 0.0061).
Conclusions
These results suggest that both quantity and quality of the skeletal muscle continued to decrease during 12-month period before death in breast cancer patients.





Similar content being viewed by others
References
Fearon K, Strasser F, Anker SD, Bosaeus I, Bruera E, Fainsinger RL, Jatoi A, Loprinzi C, MacDonald N, Mantovani G et al (2011) Definition and classification of cancer cachexia: an international consensus. Lancet Oncol 12:489–495
Geoffery H, Nathan IC, Nicholas AC, Marie F, Stein K, Russell KP (2011) Weight loss in palliative medicine. In: Oxford textbook of palliative medicine, 4th edn. Oxford University Press Inc., New York, pp 888–907
Laviano A, Meguid MM (1996) Nutritional issues in cancer management. Nutrition 12:358–371
Martin L, Birdsell L, Macdonald N, Reiman T, Clandinin MT, McCargar LJ, Murphy R, Ghosh S, Sawyer MB, Baracos VE (2013) Cancer cachexia in the age of obesity: skeletal muscle depletion is a powerful prognostic factor, independent of body mass index. J Clin Oncol 31:1539–1547
Tisdale MJ (1997) Biology of cachexia. J Natl Cancer Inst 89:1763–1773
Prado CM, Lieffers JR, McCargar LJ, Reiman T, Sawyer MB, Martin L, Baracos VE (2008) Prevalence and clinical implications of sarcopenic obesity in patients with solid tumours of the respiratory and gastrointestinal tracts: a population-based study. Lancet Oncol 9:629–635
Aust S, Knogler T, Pils D, Obermayr E, Reinthaller A, Zahn L, Radlgruber I, Mayerhoefer ME, Grimm C, Polterauer S (2015) Skeletal muscle depletion and markers for cancer cachexia are strong prognostic factors in epithelial ovarian cancer. PLoS One 10:e0140403
Sabel MS, Lee J, Cai S, Englesbe MJ, Holcombe S, Wang S (2011) Sarcopenia as a prognostic factor among patients with stage III melanoma. Ann Surg Oncol 18:3579–3585
Fujiwara N, Nakagawa H, Kudo Y, Tateishi R, Taguri M, Watadani T, Nakagomi R, Kondo M, Nakatsuka T, Minami T et al (2015) Sarcopenia, intramuscular fat deposition, and visceral adiposity independently predict the outcomes of hepatocellular carcinoma. J Hepatol 63:131–140
Villasenor A, Ballard-Barbash R, Baumgartner K, Baumgartner R, Bernstein L, McTiernan A, Neuhouser ML (2012) Prevalence and prognostic effect of sarcopenia in breast cancer survivors: the HEAL study. J Cancer Surviv 6:398–406
Prado CM, Baracos VE, McCargar LJ, Reiman T, Mourtzakis M, Tonkin K, Mackey JR, Koski S, Pituskin E, Sawyer MB (2009) Sarcopenia as a determinant of chemotherapy toxicity and time to tumor progression in metastatic breast cancer patients receiving capecitabine treatment. Clin Cancer Res 15:2920–2926
Prado CM, Sawyer MB, Ghosh S, Lieffers JR, Esfandiari N, Antoun S, Baracos VE (2013) Central tenet of cancer cachexia therapy: do patients with advanced cancer have exploitable anabolic potential? Am J Clin Nutrition 98:1012–1019
Eisenhauer EA, Therasse P, Bogaerts J et al (2009) New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 45:228–247
Mitsiopoulos N, Baumgartner RN, Heymsfield SB, Lyons W, Gallagher D, Ross R (1998) Cadaver validation of skeletal muscle measurement by magnetic resonance imaging and computerized tomography. J Appl Physiol (Bethesda, Md: 1985) 85:115–122
Shen W, Punyanitya M, Wang Z, Gallagher D, St-Onge MP, Albu J, Heymsfield SB, Heshka S (2004) Total body skeletal muscle and adipose tissue volumes: estimation from a single abdominal cross-sectional image. J Appl Physiol (Bethesda, Md: 1985) 97:2333–2338
Esfandiari N, Ghosh S, Prado CMM, Martin L, Mazurek V, Baracos VE (2014) Age, obesity, sarcopenia, and proximity to death explain reduced mean muscle attenuation in patients with advanced cancer. J Frailty Aging 3:3–8
Goodpaster BH, Kelley DE, Thaete FL, He J, Ross R (2000) Skeletal muscle attenuation determined by computed tomography is associated with skeletal muscle lipid content. J Appl Physiol (Bethesda, Md: 1985) 89:104–110
Berg HE, Tedner B, Tesch PA (1993) Changes in lower limb muscle cross-sectional area and tissue fluid volume after transition from standing to supine. Acta Physiol Scand 148:379–385
Lieffers JR, Mourtzakis M, Hall KD, McCargar LJ, Prado CM, Baracos VE (2009) A viscerally driven cachexia syndrome in patients with advanced colorectal cancer: contributions of organ and tumor mass to whole-body energy demands. Am J Clin Nutrition 89:1173–1179
van Dijk DP, Bakens MJ, Coolsen MM, Rensen SS, van Dam RM, Bours MJ, Weijenberg MP, Dejong CH, Olde Damink SW (2016) Low skeletal muscle radiation attenuation and visceral adiposity are associated with overall survival and surgical site infections in patients with pancreatic cancer. J Cachexia Sarcopenia Muscle
Srdic D, Plestina S, Sverko-Peternac A, Nikolac N, Simundic AM, Samarzija M (2016) Cancer cachexia, sarcopenia and biochemical markers in patients with advanced non-small cell lung cancer-chemotherapy toxicity and prognostic value. Suppor Care Cancer 24:4495–4502
Acknowledgments
We would like to thank Dr. Hisao Imai (Department of Respiratory Medicine, Gunma Prefectural Cancer Center), Dr. Norihiko Seki (Department of Medical Oncology, Teikyo University School of Medicine), and Dr. Satoshi Ohno, (Teikyo Academic Research Center, Teikyo University) for constructive advice regarding this study. We wish to thank Dr. Tomonori Kanda (Department of Radiology, Teikyo University School of Medicine), for technical assistance, and Dr. Kaoru Takahashi and Dr. Seiichiro Nishimura (Department of Breast Surgery, Shizuoka Cancer Center), for patient information. We greatly appreciate Dr. Tadashi Ikeda (Department of Surgery, Teikyo University School of Medicine), for the encyclopedia of breast cancer. We are particularly thankful to Dr. Kenji Eguchi (Health Science on Supportive Medicine for Intractable Disease, Teikyo University School of Medicine) for providing expertise and helping to prepare this manuscript. This study was funded by the Promotion Plan for the Platform of Human Resource Development for Cancer. The authors would like to thank Enago ( www.enago.jp) for the English language review.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
All procedures involving human participants were performed in accordance with the ethical standards of the institutional and/or national research committee and the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Kubo, Y., Naito, T., Mori, K. et al. Skeletal muscle loss and prognosis of breast cancer patients. Support Care Cancer 25, 2221–2227 (2017). https://doi.org/10.1007/s00520-017-3628-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-017-3628-5