Abstract
Objectives
To evaluate the utility of multiphase contrast-enhanced computed tomography (CT) findings alone and in combination for differentiating focal-type autoimmune pancreatitis (f-AIP) from pancreatic carcinoma (PC).
Methods
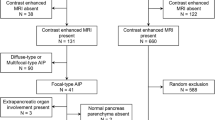
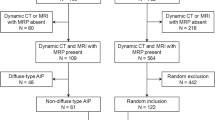
The study group comprised 22 f-AIP lesions and 61 PC lesions. Two radiologists independently evaluated CT findings. Frequencies of findings were compared between f-AIP and PC. Statistical, univariate and multivariate analyses were performed.
Results
Homogeneous enhancement during the portal phase (AIP, 59 % vs. PC, 3 %; P < 0.001), dotted enhancement during the pancreatic phase (50 % vs. 7 %; P < 0.001), duct-penetrating sign (46 % vs. 2 %; P < 0.001), enhanced duct sign (36 % vs. 2 %; P < 0.001) and capsule-like rim (46 % vs. 3 %; P < 0.001) were more frequently observed in AIP. Ring-like enhancement during the delayed phase (5 % vs. 46 %; P < 0.001) and peripancreatic strands with a length of at least 10 mm (5 % vs. 39 %; P = 0.001) were more frequently observed in PC. AIP was identified with 82 % sensitivity and 98 % specificity using four of these seven findings. Multivariate analysis revealed significant differences in dotted enhancement (P = 0.004), duct-penetrating sign (P < 0.001) and capsule-like rim (P = 0.007).
Conclusions
The combination of CT findings may allow improvements in differentiating f-AIP from PC.
Key Points
• f-AIP can mimic PC on imaging findings.
• The differentiation of f-AIP from PC is important in patient management.
• Some CT findings can be used to identify AIP.
• The combination of CT findings will improve differentiation from PC.




Similar content being viewed by others
Abbreviations
- AIP:
-
Autoimmune pancreatitis
- CBD:
-
Common bile duct
- CT:
-
Computed tomography
- f-AIP:
-
Focal-type autoimmune pancreatitis
- MPD:
-
Main pancreatic duct
- MRI:
-
Magnetic resonance imaging
- PC:
-
Pancreatic carcinoma
References
Kamisawa T, Okamoto A (2006) Autoimmune pancreatitis: proposal of IgG4-related sclerosing disease. J Gastroenterol 41:613–625
Sahani DV, Kalva SP, Farrell J et al (2004) Autoimmune pancreatitis: imaging features. Radiology 233:345–352
Kawamoto S, Siegelman SS, Hruban RH, Fishman EK (2008) Lymphoplasmacytic sclerosing pancreatitis (autoimmune pancreatitis): evaluation with multidetector CT. Radiographics 28:157–170
Yang DH, Kim KW, Kim TK et al (2006) Autoimmune pancreatitis: radiologic findings in 20 patients. Abdom Imaging 31:94–102
Weber SM, Cubukcu-Dimopulo O, Palesty JA et al (2003) Lymphoplasmacytic sclerosing pancreatitis: inflammatory mimic of pancreatic carcinoma. J Gastrointest Surg 7:129–137
Abraham SC, Wilentz RE, Yeo CJ et al (2003) Pancreaticoduodenectomy (Whipple resections) in patients without malignancy: are they all 'chronic pancreatitis'? Am J Surg Pathol 27:110–120
Kamisawa T, Shimosegawa T, Okazaki K et al (2009) Standard steroid treatment for autoimmune pancreatitis. Gut 58:1504–1507
Shimosegawa T, Chari ST, Frulloni L et al (2011) International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas 40:352–358
Okazaki K, Shimosegawa T, Itoh T et al (2012) Clinical diagnostic criteria for autoimmune pancreatitis 2011 (proposal). J Jpn Pancreas (Suizou) 27:17–25
Ghazale A, Chari ST, Smyrk TC et al (2007) Value of serum IgG4 in the diagnosis of autoimmune pancreatitis and in distinguishing it from pancreatic cancer. Am J Gastroenterol 102:1646–1653
Kamisawa T, Kim MH, Liao WC et al (2011) Clinical characteristics of 327 Asian patients with autoimmune pancreatitis based on Asian diagnostic criteria. Pancreas 40:200–205
Levy MJ, Wiersema MJ, Chari ST (2006) Chronic pancreatitis: focal pancreatitis or cancer? Is there a role for FNA/biopsy? Autoimmune pancreatitis. Endoscopy 38(Suppl 1):S30–35
Bang SJ, Kim MH, Kim Do H et al (2008) Is pancreatic core biopsy sufficient to diagnose autoimmune chronic pancreatitis? Pancreas 36:84–89
Takahashi N, Fletcher JG, Fidler JL, Hough DM, Kawashima A, Chari ST (2008) Dual-phase CT of autoimmune pancreatitis: a multireader study. AJR Am J Roentgenol 190:280–286
Takahashi N, Fletcher JG, Hough DM et al (2009) Autoimmune pancreatitis: differentiation from pancreatic carcinoma and normal pancreas on the basis of enhancement characteristics at dual-phase CT. AJR Am J Roentgenol 193:479–484
Chang WI, Kim BJ, Lee JK et al (2009) The clinical and radiological characteristics of focal mass-forming autoimmune pancreatitis: comparison with chronic pancreatitis and pancreatic cancer. Pancreas 38:401–408
Sun GF, Zuo CJ, Shao CW, Wang JH, Zhang J (2013) Focal autoimmune pancreatitis: radiological characteristics help to distinguish from pancreatic cancer. World J Gastroenterol 19:3634–3641
Irie H, Honda H, Baba S et al (1998) Autoimmune pancreatitis: CT and MR characteristics. AJR Am J Roentgenol 170:1323–1327
Suzuki K, Itoh S, Nagasaka T, Ogawa H, Ota T, Naganawa S (2010) CT findings in autoimmune pancreatitis: assessment using multiphase contrast-enhanced multisection CT. Clin Radiol 65:735–743
Kawai Y, Suzuki K, Itoh S, Takada A, Mori Y, Naganawa S (2012) Autoimmune pancreatitis: assessment of the enhanced duct sign on multiphase contrast-enhanced computed tomography. Eur J Radiol 81:3055–3060
Muhi A, Ichikawa T, Motosugi U et al (2012) Mass-forming autoimmune pancreatitis and pancreatic carcinoma: differential diagnosis on the basis of computed tomography and magnetic resonance cholangiopancreatography, and diffusion-weighted imaging findings. J Magn Reson Imaging 35:827–836
Sugiyama Y, Fujinaga Y, Kadoya M et al (2012) Characteristic magnetic resonance features of focal autoimmune pancreatitis useful for differentiation from pancreatic cancer. Jpn J Radiol 30:296–309
Fujinaga Y, Kadoya M, Hamano H et al (2011) Radiologic findings of IgG4-related disease. Curr Immunol Rev 7:186–203
Hattori Y, Gabata T, Zen Y, Mochizuki K, Kitagawa H, Matsui O (2010) Poorly enhanced areas of pancreatic adenocarcinomas on late-phase dynamic computed tomography: comparison with pathological findings. Pancreas 39:1263–1270
Morana G, Cancian L, Pozzi Mucelli R, Cugini C (2010) Staging cancer of the pancreas. Cancer Imaging 10:S137–141
Ichikawa T, Sou H, Araki T et al (2001) Duct-penetrating sign at MRCP: usefulness for differentiating inflammatory pancreatic mass from pancreatic carcinomas. Radiology 221:107–116
Zamboni G, Luttges J, Capelli P et al (2004) Histopathological features of diagnostic and clinical relevance in autoimmune pancreatitis: a study on 53 resection specimens and 9 biopsy specimens. Virchows Arch 445:552–563
Chari ST, Smyrk TC, Levy MJ et al (2006) Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin Gastroenterol Hepatol 4:1010–1016
Matsumoto S, Mori H, Kiyonaga M et al (2012) "Peripancreatic strands appearance" in pancreatic body and tail carcinoma: evaluation by multi-detector CT with pathological correlation. Abdom Imaging 37:602–608
Glaser J, Hogemann B, Krummenerl T et al (1987) Sonographic imaging of the pancreatic duct. New diagnostic possibilities using secretin stimulation. Dig Dis Sci 32:1075–1081
Takayama M, Hamano H, Ochi Y et al (2004) Recurrent attacks of autoimmune pancreatitis result in pancreatic stone formation. Am J Gastroenterol 99:932–937
Acknowledgements
The scientific guarantor of this publication is Shinji Naganawa (Department of Radiology, Nagoya University Graduate School of Medicine). The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. No complex statistical methods were necessary for this paper. Institutional review board approval was obtained. Written informed consent was waived by the institutional review board. Some study subjects or cohorts have been previously reported in 2012; Kawai Y, Suzuki K, Itoh S, et al. Autoimmune pancreatitis: assessment of the enhanced duct sign on multiphase contrast-enhanced computed tomography. Eur J Radiol 81:3055–3060. Specifically, ten focal-type autoimmune pancreatitis patients overlapped with the published study. In the previous study, only an enhancement of the main pancreatic duct wall of each patient was minutely evaluated, whereas in this study, other CT findings were additionally evaluated and regarding an enhancement of the main pancreatic duct wall, only whether present or absent was evaluated. Methodology: retrospective, diagnostic study, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Furuhashi, N., Suzuki, K., Sakurai, Y. et al. Differentiation of focal-type autoimmune pancreatitis from pancreatic carcinoma: assessment by multiphase contrast-enhanced CT. Eur Radiol 25, 1366–1374 (2015). https://doi.org/10.1007/s00330-014-3512-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3512-3