Abstract
Purpose
To determine the frequency and appearance of radiation-induced liver disease on PET/CT in patients undergoing serial imaging during neoadjuvant chemoradiation of distal esophageal cancer.
Materials and methods
In this IRB-approved, HIPAA–compliant retrospective analysis, we identified 112 patients with distal esophageal cancer treated by neoadjuvant chemoradiation who had serial PET/CT imaging available for review. Two readers reviewed all studies in consensus and recorded those cases where new foci of visually detectable increased FDG avidity appeared in the liver during therapy. The etiology of such foci was determined from corresponding findings at CT or MRI, by hepatic biopsy during surgery, by characteristic evolution on post-operative imaging, or by a combination of these methods.
Results
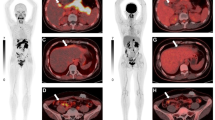
New foci of FDG avidity developed in the liver during neoadjuvant therapy in 10 of 112 (9%) patients, of whom nine (8%) were determined to have radiation-induced liver disease based on further imaging and/or biopsy and one of whom had developed interval metastatic disease based on biopsy. In the cases of radiation-induced liver disease, the abnormal foci were found only in the caudate and left hepatic lobes, near the primary tumor, while the patient who developed interval metastatic disease had involvement of the inferior right hepatic lobe, remote from the radiation therapy field.
Conclusion
New foci of increased FDG avidity are commonly seen in the caudate and left hepatic lobes of the liver during neoadjuvant chemoradiation of distal esophageal cancer, and these findings generally reflect radiation-induced liver disease rather than metastatic disease.


Similar content being viewed by others
References
Alteri R, Anderson K, Barnes C, et al. (2013). Estimated number of new cancer cases and deaths by sex, US, 2013. American Cancer Society: Cancer Facts and Figures 2013. http://www.cancer.org/research/cancerfactsstatistics/cancerfactsfigures2013/. Accessed 21 Oct 2013
Bosch DJ, Muijs CT, Mul VE, et al. (2014) Impact of Neoadjuvant Chemoradiotherapy on Postoperative Course after Curative-Intent Transthoracic Esophagectomy in Esophageal Cancer Patients. Ann Surg Oncol 21(2):605–611
Van Hagen P, Hulshof MCCM, van Lanschot JJB, et al. (2012) Preoperative chemoradiotherapy for esophageal or junctional cancer. N Engl J Med 366:2074–2084
Urschel JD, Vasan H (2003) A meta-analysis of randomized controlled trials that compared neoadjuvant chemoradiation and surgery versus surgery alone for resectable esophageal cancer. Am J Surg 185:538–543
Bosset J, Gignoux M, Triboulet J, et al. (1997) Chemoradiotherapy followed by surgery alone in squamous cell carcinoma of the esophagus. N Engl J Med 337:161–167
Bates BA, Detterbeck FC, Bernard SA, et al. (1996) Concurrent radiation therapy and chemotherapy followed by esophagectomy for localized esophageal carcinoma. J Clin Oncol 14:156–163
Donington JS, Miller DL, Allen MS, et al. (2003) Tumor response to induction chemoradiation: influence on survival after esophagectomy. Eur J Cardiothorac Surg 4:631–637
Swisher SG, Ajani JA, Komaki R, et al. (2003) Long-term outcome of phase II trial evaluating chemotherapy, chemoradiotherapy, and surgery for locoregionally advanced esophageal cancer. Int J Radiat Oncol Biol Phys 1:120–127
Kim TJ, Kim HY, Lee KW, Kim MS (2009) Multimodality assessment of esophageal cancer: preoperative staging and monitoring of response to therapy. Radiographics 29:403–421
Daly JM, Fry WA, Little AG, et al. (2000) Esophageal cancer: results of an American College of Surgeons Patient Care Evaluation Study. J Am Coll Surg 190:562–572
Bruzzi JF, Munen RF, Truong MT, et al. (2007) PET/CT of esophageal cancer: its role in clinical management. Radiographics 27:1635–1652
Levine EA, Farmer MR, Clark P, et al. (2006) Predictive value of 18-fluoro-deoxy-glucose-positron emission tomography (18F-FDG PET) in the identification of responders to chemoradiation therapy for the treatment of locally advanced esophageal cancer. Ann Surg 243:472–478
Iyer RB, Balachandran A, Bruzzi JF, et al. (2007) PET/CT and hepatic radiation injury in esophageal cancer patients. Cancer Imaging 7:189–194
Itai Y, Murata S, Kurosaki Y, et al. (1995) Straight border sign of the liver: spectrum of CT appearances and causes. Radiographics 15:1089–1102
Unger EC, Lee JKT, Weyman PJ (1987) CT and MR Imaging of Radiation Hepatitis. J Comput Assist Tomogr 11:264–268
Kawamoto S, Soyer P, Fishman EK (1998) Nonneoplastic liver disease: evaluation with CT and MR imaging. Radiographics 18:827–848
Lee JKT, Sagel SS, Stanley RJ, et al. Computed Tomography with MRI Correlation.
Willmart S, Nicaise N, Struyven J, et al. (2000) Acute radiation-induced hepatic injury: evaluation by triphasic contrast enhanced helical CT. Br J Radiol 73:544–546
Suto YS, Kato T, Yoshida K (1996) MRI Findings in Radiation-Induced Hepatic Injuries. Yonago Acta Medica 39:127–134
Yankelevitz DF, Knappp PH, Henschke Cl (1992) MR appearance of radiation hepatitis. Clin Imaging 16:89–92
Gazelle GS, Saini S, Mueller PR (1997) Hepatobiliary and Pancreatic Radiology: Imaging and Intervention. New York: Thieme Medical Publishers, Inc.; pp. 289.
Eisenberg RL (1996) Gastrointestinal radiology: a pattern approach. Hagerstown: Lippincott-Raven Publishers, p 1118
Bruzzi JF, Swisher SG, Truong MT, et al. (2007) Detection of interval distant metastases: clinical utility of integrated CT-PET imaging in patients with esophageal carcinoma after neoadjuvant therapy. Cancer 109:125–134
Quint LE, Hepburn LM, Francis IR, et al. (1995) Incidence and distribution of distant metastases from newly diagnosed esophageal carcinoma. Cancer 76:1120–1125
Mandard AM, Chasle J, Manray J, et al. (1981) Autopsy findings in 111 cases of esophageal cancer. Cancer 48:329–335
Feldman M, Friedman LS, Brandt LJ (2010) Sleisenger & Fordtran’s gastrointestinal and liver disease, 9th edn. Philadelphia: Saunders, pp 745–767
Domachevsky L, Jacene HA, Sakellis CG, Kim CK. Postradiation Changes in Tissues: Evaluation by Imaging Studies with Emphasis on Fluorodeoxyglucose-PET/Computed Tomography and Correlation with Histopathologic Findings. PET Clinics. DOI: 10.1016/j.cpet.2013.10.005. Review article (In Press Corrected Proof) 12 December 2013
Wong JJ, Anthony M-P, Khong PL (2012) Hepatic radiation injury in distal esophageal carcinoma: a case report. Clin Nucl Med 37:709–711
Nakahara T, Takagi Y, Takemasa K, et al. (2008) Dose-related fluorodeoxyglucose uptake in acute radiation-induced hepatitis. Eur J Gastroenterol Hepatol 20:1040–1044
DeLappe EM, Truong MT, et al. (2009) Hepatic radiation injury mimicking a metastasis on positron-emission tomography/computed tomography in a patient with esophageal carcinoma: a case report. J Thorac Oncol 37(7):709–711
Coakley FV, Saltavi A, Costouros NG, et al. (2011) F-18 FDG PET/CT findings in postradiation pelvic insufficiency fracture. Clin Imaging 35:139–142
Pollen JJ, Shlaer WJ (1979) Osteoblastic response to successful treatment of metastatic cancer of the prostate. Am J Roentgenol 132:927–931
Janicek MJ, Hayes DF, Kaplan WD (1994) Healing flare in skeletal metastases from breast cancer. Radiology 192:201–204
Ulaner GA, Lyall AL (2013) Identifying and distinguishing treatment effects and complications from malignancy at FDG PET/CT. Radiographics 33:1817–1834
Mettler FA, Guiberteau MJ (2012) Essentials of Nuclear Medicine, 6th edn. Philadelphia: Elsevier Saunders, pp 373–374
Acknowledgments
RAD supported by NIBIB grant 1R25EB016671.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Grant, M.J., Didier, R.A., Stevens, J.S. et al. Radiation-induced liver disease as a mimic of liver metastases at serial PET/CT during neoadjuvant chemoradiation of distal esophageal cancer. Abdom Imaging 39, 963–968 (2014). https://doi.org/10.1007/s00261-014-0125-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-014-0125-x